I have always loved children! In
KIDS CAN HAVE ARTHRITIS!
When I was younger I thought that “arthritis and autoimmune conditions” only affected adults. I realized that this is a myth while I rotated through the Pediatrics rheumatology clinic during my fellowship at NYU. I saw numerous children affected by this chronic disease, even as little as age 2. Although it was difficult at times watching these little individuals battle through days of joint pain and joint swelling as well as other systemic symptoms related to their disease or treatment, I did find it rewarding when
WHAT IS JUVENILE ARTHRITIS?
Nearly 300,000 children in America have been diagnosed with juvenile arthritis which can cause chronic arthritis in children less than sixteen years of age. This condition is an autoimmune disease where there
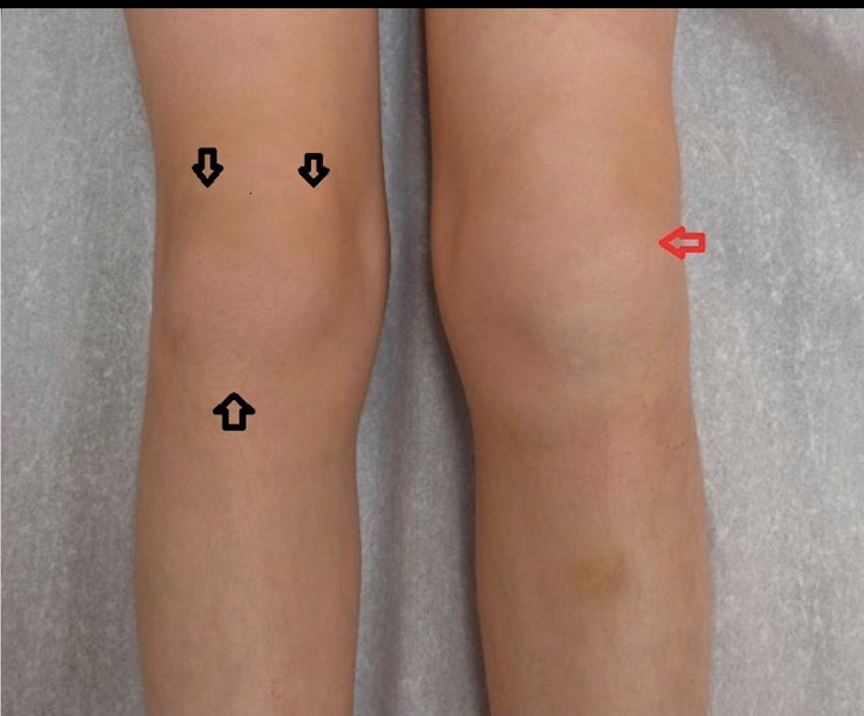

CLASSIFICATION
There are different classifications of Juvenile idiopathic arthritis (JIA) which can be based on numerous factors such as:
- Number of involved joints
- Age of onset
- Presence or absence of lab tests ( positive or negative rheumatoid factor or ANA)
- Other associated clinical features
DIFFERENT SUBTYPES
- Oligoarticular – most common form called Juvenile rheumatoid arthritis affecting fewer than 5 joints with the onset of disease (usually knees, ankle, wrist are involved)The eye can be inflamed (Iritis/Uveitis)Girls are more affected symptoms may resolve before adulthood
- Polyarticular Juvenile Idiopathic Arthritis -similar to adult RA
- Involves more than 5 joints on onset (can affect hands, feet, neck, jaw)
- There is symmetrical distribution (same affected joints on both sides)
- Girls are more affected
- Systemic Onset– Still’s Disease
- Can affect multiple organs including the liver, lymph nodes, spleen, heart
- Characterized by daily fevers (often twice a day) and diffuse rash on the arms, legs, and trunk
- Eye inflammation is NOT usually seen
- Girls and boys are affected equally
- Lab abnormalities may be seen
like increased inflammation markers (high ESR, CRP, and ferritin). High white blood cell count and platelets may be seen as well as liver abnormalities and anemia.
- Juvenile Psoriatic Arthritis
- Skin disorder, psoriasis ( with red and scaly lesions) is present
- Can occur at any age
- Back pain may be seen and other joints affected may be in an asymmetric pattern
- Nail abnormalities like nail pitting may be detected
- Enthesitis Related
- There is inflammation where the tendons attach to the bone, entheses
- Boys are usually affected
over the age of eight years old - Spine, sacroiliac joints and hips can be affected
- Sausage digits and eye inflammation can be seen
- The HLA-B27 gene test may be positive and there can be a family history of Ankylosing Spondylitis which affects the spine
NOTE: Eye (Opthalmology) screening is recommended for some subtypes of juvenile arthritis!!
It is important in children before making a diagnosis of juvenile arthritis to EXCLUDE other medical conditions such as Lyme Disease, Lupus, Bone disorders, Fibromyalgia, Infection, and Cancer.
EVALUATION
The physician evaluation will include a complete history and physical examination and possibly these tests:
- Xrays
- MRI scans
- Lab tests (compelte blood count, rheumatoid factor, antinuclear antibody test)
- Tests for infections ( blood culture and other viral tests)
- Possible bone marrow exam to look for leukemia
- Joint fluid analysis if swelling is present
- Bone scan
Treatment Options
The goal is to reduce joint pain and swelling, prevent joint damage, and increase joint mobility
- Nonsteroidal anti-inflammatory drugs (NSAIDs)- like Naproxen and Ibuprofen
- Can help reduce pain and swelling
- Nausea, abdominal pain, bruising may be seen as side effects
- Steroids
Disease Modifying Agents (DMARDs)- Methotrexate
- Hydroxychloroquine (Plaquenil)
- Sulfasalazine (Azulfidine)
- Biologic injections (Anti TNF medication- blocks a certain chemical TNF which causes systemic and joint inflammation
- Etanercept
- Adalimumab
- Infliximab
- Anakinra
It is important to recognize that parents and physician need to address the emotional and social effects of the disease and find support for the children. Psychological counseling and organizations like the Arthritis Foundation are available!
There are also other autoimmune diseases that affect children such as lupus, dermatomyositis, scleroderma, mixed connective tissue disease, and fibromyalgia.
Kawasaki disease is another childhood autoimmune disease causing inflammation of the blood vessels and heart complications such as aneurysms.
To all the children out in the world fighting arthritis and autoimmune diseases, you are all champions! Keep fighting with your spirit!!
Reference: Current Diagnosis and TreatmentRheumatology
Disclaimer: This blog contains my personal opinion based on personal and clinical experience, tips from trainers, health coaches and lastly research. This blog does not endorse specific treatments, procedures, products. You should always consult with a doctor, nutritionist, or other healthcare professional to discuss your own health and lifestyle goals and regimen based on your medical history. Thank you for reading!
