ARTHRITIS HITS CLOSE TO HOME
Psoriatic arthritis (PsA) is a type of arthritis associated with inflammation that can be seen with psoriasis, an autoimmune condition where patches of red skin and silvery scales may be seen. This type of arthritis which may appear before or after the skin lesions, can resemble rheumatoid arthritis.
I remember the first time I saw someone with psoriatic arthritis. It was during my high school years. When I think back to that period, I remember watching my best friend’s father who is a physician battle with daily joint pain, stiffness and swelling. He had psoriasis for many years in his young adulthood but his joint symptoms started when he was thirty eight. His symptoms progressed for several years where he had difficulty with walking and prolonged standing because of joint inflammation. As time went on, his skin disease also became worse.
I remember being amazed that how such a young person could suffer such a debilitating disease. I spent a lot of time at my friend’s house so I was able to personally witness the slow deterioration of his function over thirteen years until he could not function at work anymore and keep up wit of his daily hectic schedule at the medical practice and hospital rounds. He had to temporarily walk away from his medical practice for several years until his physical function improved after receiving medication.
OTHER STORIES
I once took care of young woman in her thirties who came in the office because she experienced joint pain, stiffness in her low back as well as intermittent swelling in her hands, wrists, knees and ankles for several years. She had noticed joint pain on and off for years which got better during her first pregnancy. When she came to me, after the delivery of her child, she noted some hand deformities and “locking” in one hand. She also noticed that her psoriasis on her scalp, knees, elbows and shin got much worse after the birth of her child.
She complained of not being able to pick up her baby or do simple things like changing diapers, twisting the caps to bottles or lifting the baby due to the pain and swelling. Imagine not being able to hold a child due to arthritis? She wanted to get pregnant again quickly but had some reservations due to her fatigue and chronic pain.
Many golf fans know that Phil Mickelson, one of golf’s top icons has also talked openly about his struggle with psoriatic arthritis since the 2010 US Open Championship at Pebble Beach. He has continuously expressed his desire to stay on top of his game on and off the course. I can imagine how difficult it is to play a sport and manage a career which requires so much twisting, bending, gripping and swinging while battling inflammation.
WHAT IS PSORIATIC ARTHRITIS?
PSORIATIC ARTHRITIS? is a chronic disease associated with inflammation of the skin and joints. Often the psoriasis may appear before the onset of the arthritis, however the joint pain may precede the skin inflammation which may occur in areas such as the elbows, ears, scalp, stomach and around the genital areas. According to the National Psoriasis Foundation between ten and thirty percent of people with psoriasis develop psoriatic arthritis.
There are five types of psoriatic arthritis: symmetrical with multiple joints involvement, asymmetrical with few joints involvement, spine involvement, complete distal digits/toe swelling (dactylitis), and a very destructive and deforming type causing irreversible joint damage (mutilans).
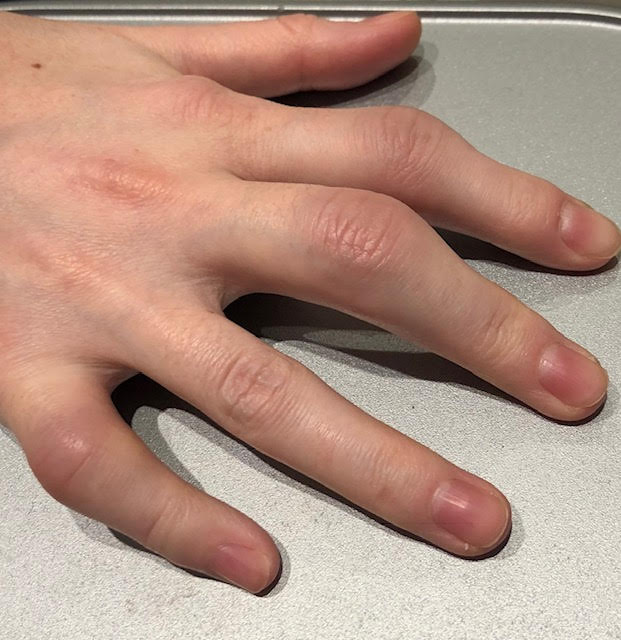
RISK FACTORS
The cause of this systemic disease is unknown. There are risk factors that can promote the development of PsA.
– Having psoriasis
– Family History of someone with psoriasis
– Age (usually in middle age from 30s to 50s). It can also happen earlier in life as well.
– HLA B27 gene marker found in the blood can be seen with psoriatic arthritis involving the spine
– Stress can trigger the immune system
– There are theories of possible trauma or viral and bacterial infection possibly stimulating psoriasis in people with a genetic or hereditary predisposition
DISTINGUISHING FEATURES OF PSORIATIC ARTHRITIS
a) Swelling of the entire digits/fingers or toes (sausage digits)
b) Spinal involvement (spondylitis) or involvement of the area between the spine and pelvis (sacroilitis)
c) Discoloration or disorder of the nail beds (nail pitting/ridging of finger and toenails)
d) Inflammation of the areas where the tendons and ligaments attach to the bones (enthesitis). Often the Achilles tendon or elbow tendon may be involved (Achilles tendonitis, epicondylitis). The soles of the feet can also have soreness (plantar fasciitis).
e) Chest wall irritation (costochondritis)
DIAGNOSIS
A rheumatologist will do a thorough physical examination of joints, tendons, and fingernails. The physician may order radiographs, ultrasound and MRI to look for damage to the joints and soft tissues in the body. Laboratory tests such as inflammation markers and blood test for genetic marker HLA-B27 may be ordered. If a joint has significant swelling, joint fluid may be removed from the joint for analysis. It is important to have a dermatologist, physical therapist and possibly other specialists involved in management.
MEDICAL TREATMENT
It is always important to remember that there is no cure for this disease but there are treatments to help individuals live a fulfilled life, although it may take time to get to that point.
1) Nonsteroidal anti-inflammatory drugs (NSAIDS) such as Naproxen or Ibuprofen
2) Disease Modifying Antirheumatic Drugs DMARDs) – Methotrexate, Sulfasalazine can help slow the progression of damage.
3) Steroids (oral or injections)
3) Biologics- These medications block certain chemicals that can cause inflammation and joint damage.
-Etanercept (Enbrel)
-Adalimumab (Humira)
-Golimumab (Simponi)
-Certolizumab Pegol (Cimzia)
-Infliximab (Remicade)
4) Newer medications which block certain chemicals or key components of the inflammation pathway to treat psoriasis and reduce joint symptoms include:
– Ustekinumab (Stelara)
– Secukinumab (Cosentyx)
-Apremilast (Otezela)
There are so many options. Phototherapy and other immunosuppressants can also be used for psoriasis.
Please review these options with your physician based on personal medical history and risk factors. There are increased risk of infection with these medications and tuberculosis as well as Hepatitis B and C screeningis necessary.
PSORIATIC ARTHRITIS COMPLICATIONS
Like many inflammatory arthritis, the joints are not the only affected parts of the body. Other organs can be affected such as the eyes, lungs, gastrointestinal tract/bowel and the largest blood vessel, the aorta. There is an increased risk of heart disease in these individuals!
LIFESTYLE TIPS
Incorporate a healthy diet of fruits, vegetables, omega-3 fatty acids and maintain a healthy weight.
-Relax and reduce stress
-Keep joints flexible by maintaining an exercise regimen that is not too taxing (swimming, yoga).
-Consider incorporating more vitamin D in diet which may help with skin and joint symptoms. There are studies that have reviewed the role that vitamin D plays in the regulation of the immune system.
MOVING ON
Phil Mickelson has gone on to win tournaments despite living with this chronic debilitating condition. He credits his ability to keep doing what he loves and spending time with his family due to early and aggressive treatment. My friend’s father eventually went on several treatments and returned back to clinical practice. It is still a struggle on some days to move and work long physician hours but he is living a productive life.
Like other chronic medical conditions such as Diabetes and Hypertension, management of Psoriatic Arthritis may be difficult for patients and their loved ones. Some patients may develop depression and issues with self-esteem and intimacy from the emotional impact of the skin disease and joint restriction. Social activities and engagement may be avoided due to challenges with mobility and extreme fatigue due to decrease sleep. It is crucial to have a strong support network of family, friends, health care practitioners and a therapist.
For more information, please check out:
National Psoriasis Foundation (www.psoriasis.org)
Arthritis Foundation (www.arthritis.org)
References:
Psoriasis Forum 2010 Winter, 16(4) 17-25
Journal of European Academy Dermatology Venerol.2010; 24, Supplement 2, 31-5
New England Journal of Medicine. 2007; 357:266-81
Arthritis Research and Therapy. 2008; 10:123
Current Diagnosis in Rheumatology Second edition
Disclaimer: This information is for educational purposes only, not as medical advice or as a diagnosis. This blog contains my personal opinion based on personal and clinical experience, tips from trainers, health coaches and lastly research. You should always consult with a doctor, nutritionist, or other healthcare professional to discuss your own health and lifestyle goals and regimen based on your medical history. Please see your physician should you have any questions, symptoms, or any concerns. Thank you for reading!

